Introduction
Pemphigus vulgaris (PV) is a potentially life-threatening autoimmune blistering disorder caused by antibodies against desmoglein 1 and 3, resulting in intraepidermal acantholysis. In clinical practice, fragile bullae may rupture quickly, leaving painful erosions involving skin and mucosa.
This case demonstrates successful management of erosive-phase pemphigus vulgaris using dexamethasone-cyclophosphamide pulse therapy (DCP), topical care, and structured supportive management.
Case Presentation
A 65-year-old female presented with painful, progressive erosions over abdomen, trunk, and lower limbs for 3-4 weeks. Lesions began as fragile blisters and rapidly converted into raw, oozing erosions.
- Severe burning pain and skin tenderness
- Mobility limitation due to painful erosions
- Oral ulcerations causing painful oral intake
- Positive Nikolsky sign
- No intact fluid-filled blisters at presentation
Diagnostic Approach
- Clinical diagnosis based on erosions, mucosal involvement, and Nikolsky positivity
- Serology: anti-desmoglein (Dsg1 and Dsg3) antibodies positive
- Supportive histopathology findings when performed: intraepidermal acantholysis and intercellular IgG deposition in fish-net pattern
Differentials considered: bullous pemphigoid, Stevens-Johnson syndrome, toxic epidermal necrolysis, and drug-induced blistering disorders.
Pathophysiology
In PV, pathogenic IgG autoantibodies against desmoglein molecules disrupt keratinocyte adhesion, causing acantholysis and intraepidermal blistering. Mucosal disease is strongly associated with anti-Dsg3 antibodies. Because erosions can rapidly expand and compromise barrier function, early systemic immunosuppression is critical.
Treatment Approach
Primary Systemic Therapy
- Injectable dexamethasone pulse therapy
- Cyclophosphamide as concomitant immunosuppressive therapy
The DCP regimen was chosen to quickly suppress disease activity, reduce autoantibody production, and promote re-epithelialization.
Adjunctive and Supportive Care
- Topical corticosteroids over erosive lesions
- Topical and oral antibiotics for infection prevention and control
- Regular non-adherent dressings and gentle cleansing
- High-protein nutrition with hydration and electrolyte support
- Oral lesion protocol with pain-control and mucosal healing support
Clinical Course
- 2-3 weeks: marked reduction in new lesion formation
- Progressive healing of erosions with lower exudation
- Improvement in oral erosions and oral intake tolerance
Additional Treatment Modalities
Depending on severity and response, further options in PV include oral corticosteroids, azathioprine, mycophenolate mofetil, methotrexate, rituximab, IVIG, and plasmapheresis. In this patient, early DCP initiation achieved control and reduced escalation needs.
Clinical Implications
- PV may present primarily as erosions when bullae rupture before evaluation
- Serology helps early confirmation when morphology is atypical
- Comprehensive wound care and infection prevention are central to outcomes
- Early aggressive treatment can prevent progression and systemic complications
Before and After
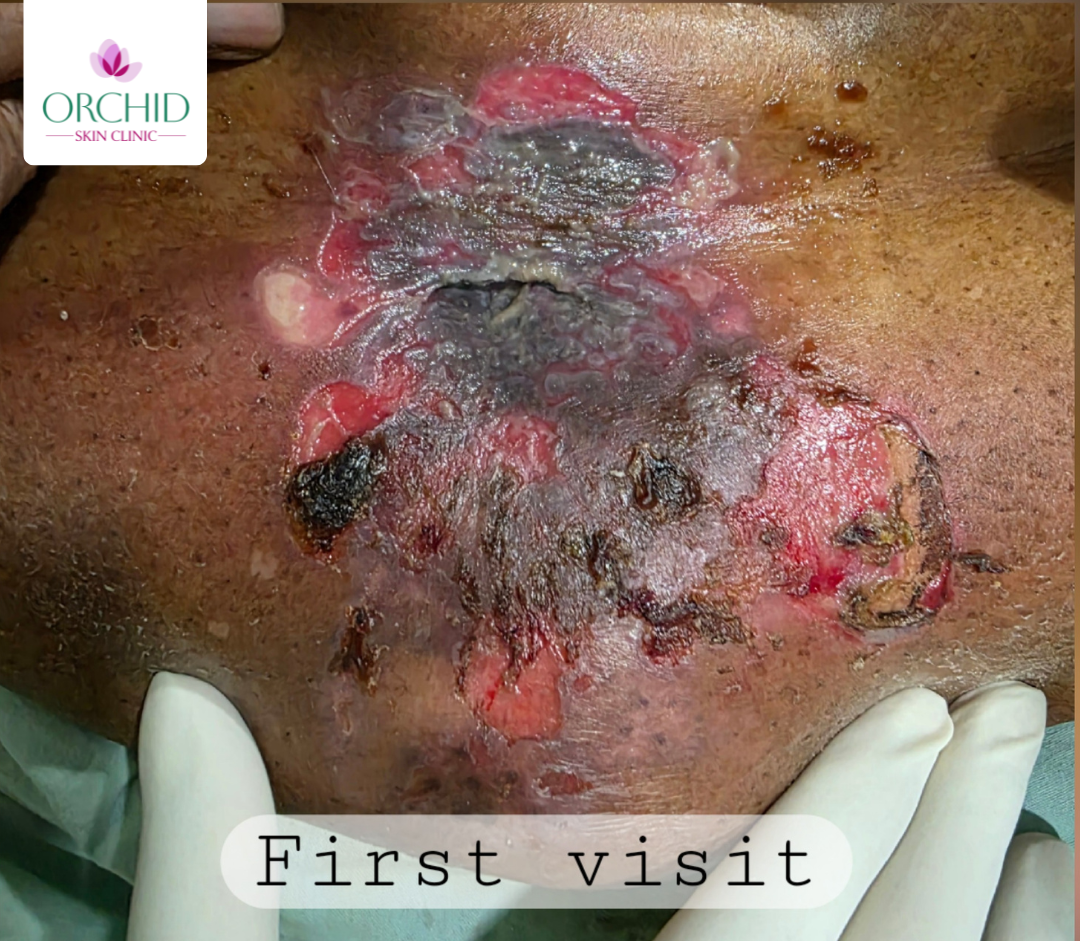
Before Treatment
Suggested image: extensive erosions with active disease over trunk or limbs prior to pulse therapy initiation.
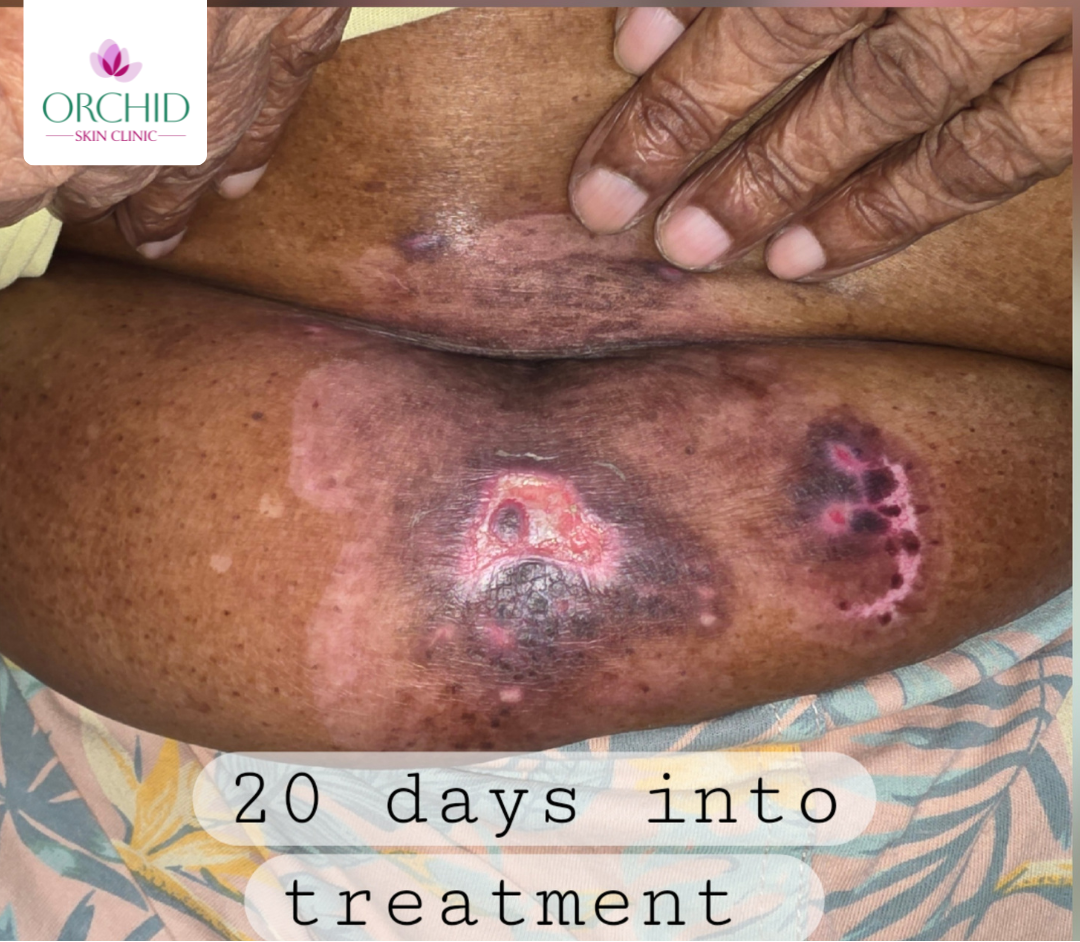
After DCP Pulse Therapy
Suggested image: re-epithelialization and reduced erosive burden after systemic control and structured wound care.
Replace the placeholders above with the final before/after clinical photographs once available.
Conclusion
This case highlights successful treatment of erosive pemphigus vulgaris with dexamethasone-cyclophosphamide pulse therapy integrated with local wound management and systemic supportive care. Timely diagnosis and multidisciplinary treatment remain essential to reduce morbidity in autoimmune blistering disease.