Tissue necrosis after a skin biopsy is uncommon, but risk rises in pressure bearing areas like the plantar foot. Early recognition and timely surgical intervention are critical to prevent deeper tissue involvement and prolonged morbidity.
This case highlights successful management of a necrotic post-biopsy wound using surgical debridement and structured wound care.
Case Presentation
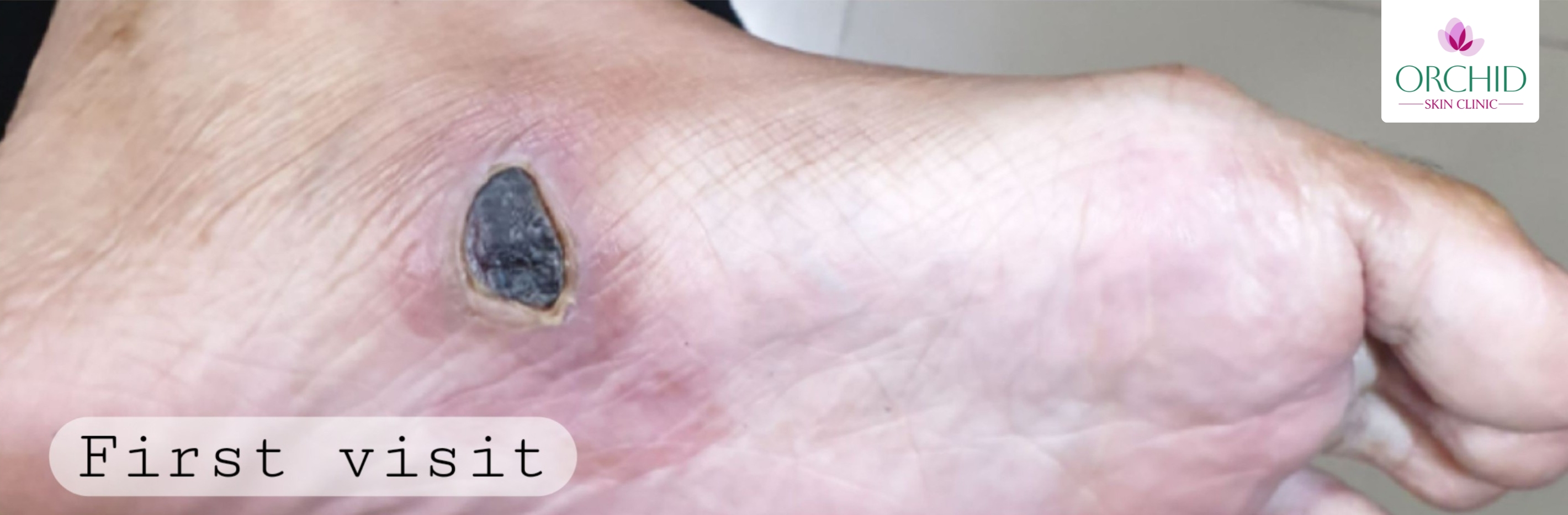
A 20-year-old female presented with a painful, blackish lesion over the plantar aspect of the left foot at the site of a biopsy performed around two weeks earlier for evaluation of a pigmented lesion.
The patient reported:
- Increasing pain on weight bearing
- Dark discoloration of the biopsy site
- Mild surrounding redness
- No systemic symptoms such as fever
On examination:
- Well demarcated necrotic eschar measuring about 1.5 to 2 cm by 2 cm
- Surrounding mild erythema and induration
- No overt purulent discharge
- Peripheral pulses palpable and intact
- No sensory deficit
Diagnostic Approach
Diagnosis was primarily clinical, supported by characteristic black eschar formation and local tenderness with no systemic toxicity.
Differential diagnoses considered:
- Post biopsy infection
- Hematoma with secondary necrosis
- Vasculitic ulcer
- Pressure induced ischemic ulcer
Baseline investigations included CBC and blood glucose. Doppler was not required because peripheral perfusion was clinically adequate.
Pathophysiology
Post procedural necrosis can occur due to compromised local blood supply, excessive cautery, secondary infection, pressure related ischemia, or inflammatory vascular compromise. The plantar foot is vulnerable due to constant mechanical stress and limited soft tissue padding.
Treatment Approach
Primary Intervention: Surgical Debridement
- Local anesthesia administered under aseptic precautions
- Complete removal of necrotic eschar
- Non viable tissue sharply debrided
- Wound bed assessed for viable granulation tissue
- Hemostasis achieved
Debridement converted the wound from a necrotic, non healing state into a clean, vascular wound bed conducive to healing.
Key Clinical Point
Early debridement in pressure bearing sites prevents deeper tissue involvement and reduces infection risk.
Post Operative Medical Management
- Topical Megaheal (growth factor based wound healing agent)
- Topical fusidic acid to prevent secondary infection
- Tab. Enzoflam for pain and inflammation control
- Cap. Amoxycillin clavulanic acid as prophylactic antibiotic
- Strict regular dressing protocol
- Weight off loading and limited pressure
Follow-Up Progress
Healing proceeded without secondary infection or need for advanced surgical intervention.
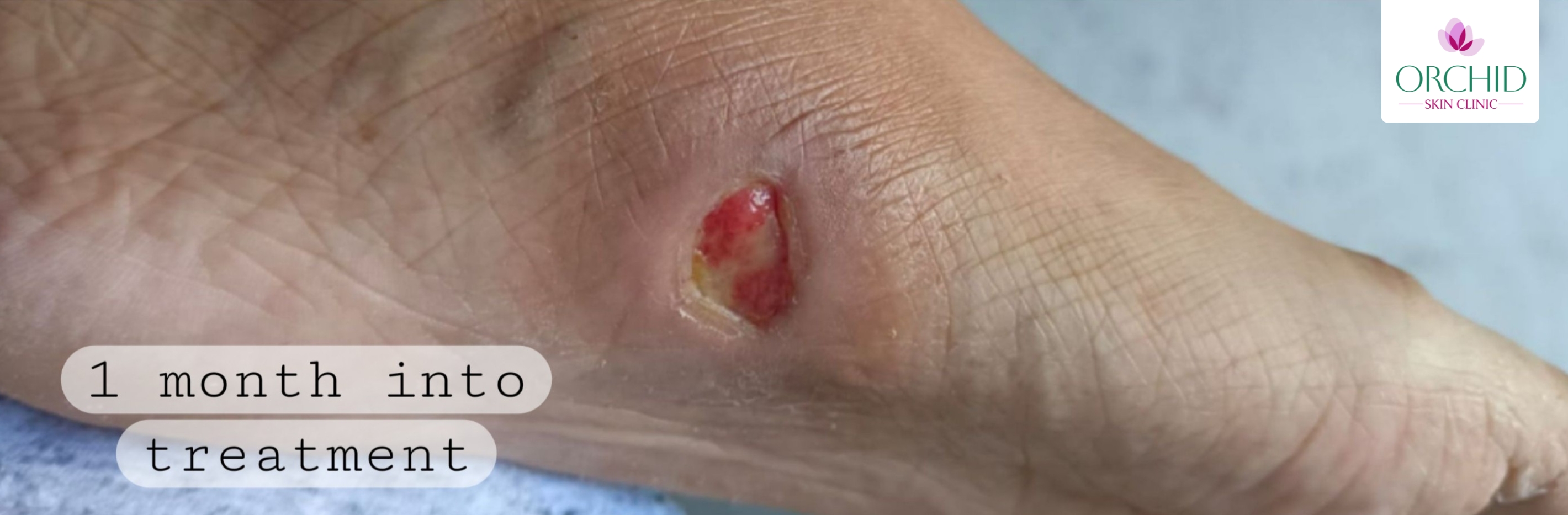
- 1 Month: Healthy granulation tissue with progressive epithelialization
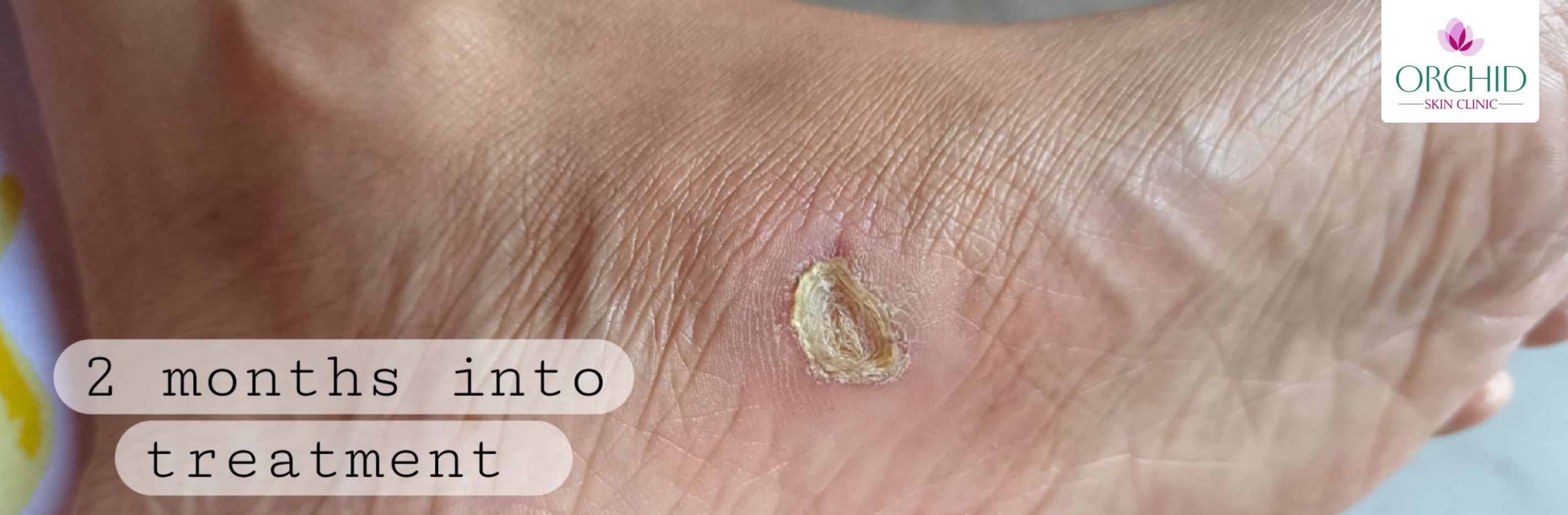
- 2 Months: Significant reduction in wound size with dry scab formation and no signs of infection
Additional Treatment Modalities Considered
Depending on severity and response, alternatives may include:
- Advanced wound dressings (hydrocolloid, alginate, foam)
- Negative pressure wound therapy
- Platelet rich plasma for non healing wounds
- Topical silver based antimicrobial dressings
- Surgical revision or flap coverage
- Hyperbaric oxygen therapy in ischemic cases
Clinical Implications
- Monitor biopsy sites in pressure bearing areas closely
- Recognize early ischemic changes promptly
- Debridement and structured wound care improve outcomes
- Off loading is critical for plantar wounds
Conclusion
A 20-year-old female with localized post-biopsy tissue necrosis of the plantar foot was successfully managed with timely surgical debridement and structured wound care, resulting in progressive healing without complications.
This case underscores the importance of early intervention, proper off loading, and disciplined follow up in high pressure anatomical regions.
Concerned About a Non Healing Wound?
A professional evaluation can help determine the right treatment approach.
Schedule Your ConsultationWhy can plantar biopsy sites heal slowly?
Plantar skin is exposed to constant pressure and shear, which can delay healing and worsen ischemic changes.
When is surgical debridement needed?
Debridement is indicated when non viable tissue is present and the wound is not progressing toward healing.
How long can healing take?
Mild to moderate wounds may improve within 1 to 2 months with proper care and off loading.